"Screw You: If we cant make money - you're dead"
May 27, 2020 23:04:05 GMT 10
brillbilly and Rareclan like this
Post by Deleted on May 27, 2020 23:04:05 GMT 10
Taxpayers paid to develop remdesivir but will have no say when Gilead sets price
Christopher Rowland, The Washington Post
Tuesday, May 26, 2020
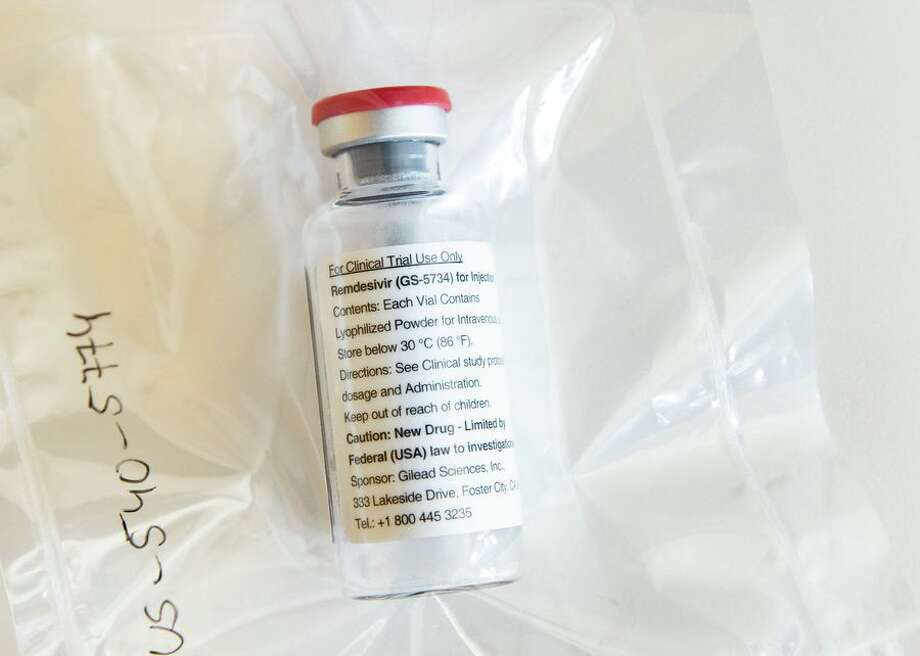
Photo: CBSI/CNET
- One drug that has shown promise for treating COVID-19 is remdesivir, an experimental antiviral product from Gilead Sciences. On April 29, the US National Institute of Allergy and Infectious Diseases said that preliminary data from a US-based clinical trial showed remdesivir can help patients recover more quickly. Dr. Anthony Fauci, the director of the National Institute of Allergy and Infectious Diseases, said the early results are "a very important proof-of-concept."
The drug that buoyed expectations for a coronavirus treatment and drew international attention for Gilead Sciences, remdesivir, started as a reject, an also-ran in the search for antiviral drugs. Its path to relevance did not begin until Robert Jordan cleared it.
A Gilead scientist at the time, Jordan convinced the company seven years ago to let him assemble a library of 1,000 castoff molecules in a search for medicines to treat emerging viruses. Many viral illnesses threaten human health but do not attract commercial interest, because they lack potential for huge drug sales.
"I kept asking them, 'Is this OK?' " said Jordan, who is now a vice president at a pharmaceutical start-up. "These don't represent a commercial opportunity but a public health opportunity. Gilead gave me their blessing to do this on the side."
To make progress, Gilead needed help from U.S. taxpayers. Lots of help. Three federal health agencies were deeply involved in remdesivir's development every step of the way, providing tens of millions of dollars of government research support. Now that big government role has set up a political showdown over pricing and access.
Despite the heavy subsidies, federal agencies have not asserted patent rights to Gilead's drug, potentially a blockbuster therapy worth billions of dollars. That means Gilead will have few constraints other than political pressure when it sets a price in coming weeks. Critics are urging the Trump administration to take a more aggressive approach.
"Without direct public investment and tax subsidies, this drug would apparently have remained in the scrap heap of unsuccessful drugs," Rep. Lloyd Doggett, D-Texas, chairman of the House Ways and Means health subcommittee, said this month. Doggett and Rep. Rosa DeLauro, D-Conn., have asked Health and Human Services Secretary Alex Azar for a detailed financial accounting of federal support for remdesivir's discovery and development.
The HIV-prevention advocacy group PrEP4All Collaboration, working with the Technology Law & Policy Clinic at New York University, released an analysis Monday that said the government, because it helped cull the drug from hundreds of compounds, probably has a legal right to claim it co-invented remdesivir. It contends that government scientists should have been listed as co-inventors on remdesivir patents because of their contributions. It says the Trump administration should be leveraging the government's involvement to ensure that the United States and other countries can get access at a low cost.
"Agencies can't just punt it over the fence to a pharmaceutical company and walk away," said James Krellenstein, a co-founder of PrEP4All. "For the federal government to just walk away from that responsibility is a dereliction of the public trust."
Two other nonprofit watchdog groups, Knowledge Ecology International and Public Citizen, also have documented the large taxpayer-funded contributions toward the drug. Public Citizen estimates public investment at a minimum of $70 million.
"Gilead did not make this drug alone. The public helped make it, and the public has a stake," said Peter Maybarduk, director of the access to medicines program at Public Citizen.
Gilead has acknowledged the large role of government agencies in remdesivir's development but said that the original compound was discovered by Gilead researchers years earlier and that the government has no potential patent rights to the drug. It has said it will spend up to $1 billion on remdesivir manufacturing and development in 2020 as it rapidly increases production and distribution around the world.
"We are focused on getting this treatment into the hands of as many patients as possible and making sure it is both accessible and affordable to patients in the United States and around the globe," company spokesman Ryan McKeel said in an email. "We take that responsibility to patients and families affected by covid-19 very seriously and we will work to make sure access is not an issue.
"Gilead researchers invented remdesivir more than a decade ago, identified its broad-spectrum antiviral activity, optimized the formulation of the product and scaled up the manufacturing process," McKeel said. "Although government funding was used to further characterize remdesivir's profile after its initial discovery, this did not result in the creation of the underlying intellectual property invented by Gilead."
The story of the drug's creation shows that Gilead would not be commercializing the drug if it were not for the extensive involvement of government scientists and agencies. The industry-government partnership crossed the finish line this month when the Food and Drug Administration issued an emergency use authorization clearing remdesivir to treat hospitalized patients with covid-19, the disease caused by the coronavirus.
Screening a huge number of chemicals for effective drugs is arduous work and often fails to produce a winner. In remdesivir's case, government researchers narrowed the search from 1,000 compounds to the chemical that would become remdesivir, confirmed its potency in laboratory tests, tested it in monkeys, and finally sponsored a pivotal clinical trial in humans.
Jordan sent Gilead's screening library to the Centers for Disease Control and Prevention in Atlanta, and to Fort Detrick in Frederick, Maryland, home to the U.S. Army Medical Research Institute of Infectious Diseases (USAMRIID). Scientists at both federal facilities study dangerous viruses in high-security biocontainment labs. The National Institutes of Health and academic labs in Tennessee and North Carolina that receive NIH grants also would play key roles studying the drug in mice.
Front-line government scientists who worked directly with Gilead on the drug described the heavy involvement of federal resources in the drug's development, though they said their concern at the time was not patents but speeding treatments in the battle against dangerous diseases, especially Ebola.
The former chief scientific officer at USAMRIID who supervised the development of remdesivir, Sina Bavari, said the team was working rapidly on a treatment for Ebola in 2014 and did not consider filing a patent application when the agency's scientists helped discover new uses of the drug and tested it in government monkeys. Bavari and other government scientists were co-authors of an article in the scientific journal Nature that described its discovery and successful tests in the government's rhesus monkeys.
Gilead contributed the drug and spent millions from its own budgets to hone the drug's formulation, said Bavari, who now runs his own consulting company. Deciding when to file a government patent in the case of industry partnerships presents a "tightrope" for public health agencies that want to maintain positive relationships with industry partners, Bavari said.
Many antiviral drugs are taken for a short time and given to relatively few people. They do not represent large markets, so government subsidies are used to keep corporations interested in pursuing treatments, he said.
"Without incentivizing some of these companies to stay attached to emerging disease, I think they will walk away, even after this one," he said. "In this situation [filing for a government patent] would have caused more harm with Gilead and not been worth it.
"The government's job is to make sure industry is successful, and if industry is successful, then we all benefit from it."
An Army lawyer said the Gilead drug did not meet the threshold of a government co-invention.
"Although USAMRIID performed extensive and critical screening and testing for Gilead, testing a compound and finding that it is indeed an effective antiviral compound does not qualify USAMRIID as a joint inventor of the compound," Leigh Callander, chief patent counsel for the U.S. Army Medical Research and Development Command, said in an email.
An independent organization that measures the cost-effectiveness of drugs said Gilead could be justified in charging up to $4,500 for a 10-day course of treatment for a single coronavirus patient. But advocates, citing a study by academic researchers on what it costs to make the drug, have said Gilead could break even by charging $1 per dose.
The Department of Health and Human Services, in response to emailed questions, said it was too early to discuss pricing of remdesivir but noted that the government has reimbursed hospitals and other providers for the costs of testing and treating people with no health insurance. For those with insurance, many insurance companies have waived patient co-payments for covid-19-related care and therapies, it said.
"The Trump Administration is committed to ensuring Americans have access to life-saving therapeutics and vaccines as we combat this pandemic," it said.
Gilead is donating the first 1.5 million doses to governments worldwide, which it said was enough for at least 140,000 patients through the end of May. More than half of that was targeted for U.S. patients. The drug is given intravenously in the hospital for five to 10 days. Gilead is investigating ways of making the drug in pill form, which could dramatically increase use - and sales - especially if the coronavirus lasts for years in the human population.
FULL ARTICLE @ THE HOUSTON CHRONICLE (via Washington Post)
www.chron.com/business/article/Taxpayers-paid-to-develop-remdesivir-but-will-15296173.php
(This article could be moved under coronavirus)
Christopher Rowland, The Washington Post
Tuesday, May 26, 2020

Photo: CBSI/CNET
- One drug that has shown promise for treating COVID-19 is remdesivir, an experimental antiviral product from Gilead Sciences. On April 29, the US National Institute of Allergy and Infectious Diseases said that preliminary data from a US-based clinical trial showed remdesivir can help patients recover more quickly. Dr. Anthony Fauci, the director of the National Institute of Allergy and Infectious Diseases, said the early results are "a very important proof-of-concept."
The drug that buoyed expectations for a coronavirus treatment and drew international attention for Gilead Sciences, remdesivir, started as a reject, an also-ran in the search for antiviral drugs. Its path to relevance did not begin until Robert Jordan cleared it.
A Gilead scientist at the time, Jordan convinced the company seven years ago to let him assemble a library of 1,000 castoff molecules in a search for medicines to treat emerging viruses. Many viral illnesses threaten human health but do not attract commercial interest, because they lack potential for huge drug sales.
"I kept asking them, 'Is this OK?' " said Jordan, who is now a vice president at a pharmaceutical start-up. "These don't represent a commercial opportunity but a public health opportunity. Gilead gave me their blessing to do this on the side."
To make progress, Gilead needed help from U.S. taxpayers. Lots of help. Three federal health agencies were deeply involved in remdesivir's development every step of the way, providing tens of millions of dollars of government research support. Now that big government role has set up a political showdown over pricing and access.
Despite the heavy subsidies, federal agencies have not asserted patent rights to Gilead's drug, potentially a blockbuster therapy worth billions of dollars. That means Gilead will have few constraints other than political pressure when it sets a price in coming weeks. Critics are urging the Trump administration to take a more aggressive approach.
"Without direct public investment and tax subsidies, this drug would apparently have remained in the scrap heap of unsuccessful drugs," Rep. Lloyd Doggett, D-Texas, chairman of the House Ways and Means health subcommittee, said this month. Doggett and Rep. Rosa DeLauro, D-Conn., have asked Health and Human Services Secretary Alex Azar for a detailed financial accounting of federal support for remdesivir's discovery and development.
The HIV-prevention advocacy group PrEP4All Collaboration, working with the Technology Law & Policy Clinic at New York University, released an analysis Monday that said the government, because it helped cull the drug from hundreds of compounds, probably has a legal right to claim it co-invented remdesivir. It contends that government scientists should have been listed as co-inventors on remdesivir patents because of their contributions. It says the Trump administration should be leveraging the government's involvement to ensure that the United States and other countries can get access at a low cost.
"Agencies can't just punt it over the fence to a pharmaceutical company and walk away," said James Krellenstein, a co-founder of PrEP4All. "For the federal government to just walk away from that responsibility is a dereliction of the public trust."
Two other nonprofit watchdog groups, Knowledge Ecology International and Public Citizen, also have documented the large taxpayer-funded contributions toward the drug. Public Citizen estimates public investment at a minimum of $70 million.
"Gilead did not make this drug alone. The public helped make it, and the public has a stake," said Peter Maybarduk, director of the access to medicines program at Public Citizen.
Gilead has acknowledged the large role of government agencies in remdesivir's development but said that the original compound was discovered by Gilead researchers years earlier and that the government has no potential patent rights to the drug. It has said it will spend up to $1 billion on remdesivir manufacturing and development in 2020 as it rapidly increases production and distribution around the world.
"We are focused on getting this treatment into the hands of as many patients as possible and making sure it is both accessible and affordable to patients in the United States and around the globe," company spokesman Ryan McKeel said in an email. "We take that responsibility to patients and families affected by covid-19 very seriously and we will work to make sure access is not an issue.
"Gilead researchers invented remdesivir more than a decade ago, identified its broad-spectrum antiviral activity, optimized the formulation of the product and scaled up the manufacturing process," McKeel said. "Although government funding was used to further characterize remdesivir's profile after its initial discovery, this did not result in the creation of the underlying intellectual property invented by Gilead."
The story of the drug's creation shows that Gilead would not be commercializing the drug if it were not for the extensive involvement of government scientists and agencies. The industry-government partnership crossed the finish line this month when the Food and Drug Administration issued an emergency use authorization clearing remdesivir to treat hospitalized patients with covid-19, the disease caused by the coronavirus.
Screening a huge number of chemicals for effective drugs is arduous work and often fails to produce a winner. In remdesivir's case, government researchers narrowed the search from 1,000 compounds to the chemical that would become remdesivir, confirmed its potency in laboratory tests, tested it in monkeys, and finally sponsored a pivotal clinical trial in humans.
Jordan sent Gilead's screening library to the Centers for Disease Control and Prevention in Atlanta, and to Fort Detrick in Frederick, Maryland, home to the U.S. Army Medical Research Institute of Infectious Diseases (USAMRIID). Scientists at both federal facilities study dangerous viruses in high-security biocontainment labs. The National Institutes of Health and academic labs in Tennessee and North Carolina that receive NIH grants also would play key roles studying the drug in mice.
Front-line government scientists who worked directly with Gilead on the drug described the heavy involvement of federal resources in the drug's development, though they said their concern at the time was not patents but speeding treatments in the battle against dangerous diseases, especially Ebola.
The former chief scientific officer at USAMRIID who supervised the development of remdesivir, Sina Bavari, said the team was working rapidly on a treatment for Ebola in 2014 and did not consider filing a patent application when the agency's scientists helped discover new uses of the drug and tested it in government monkeys. Bavari and other government scientists were co-authors of an article in the scientific journal Nature that described its discovery and successful tests in the government's rhesus monkeys.
Gilead contributed the drug and spent millions from its own budgets to hone the drug's formulation, said Bavari, who now runs his own consulting company. Deciding when to file a government patent in the case of industry partnerships presents a "tightrope" for public health agencies that want to maintain positive relationships with industry partners, Bavari said.
Many antiviral drugs are taken for a short time and given to relatively few people. They do not represent large markets, so government subsidies are used to keep corporations interested in pursuing treatments, he said.
"Without incentivizing some of these companies to stay attached to emerging disease, I think they will walk away, even after this one," he said. "In this situation [filing for a government patent] would have caused more harm with Gilead and not been worth it.
"The government's job is to make sure industry is successful, and if industry is successful, then we all benefit from it."
An Army lawyer said the Gilead drug did not meet the threshold of a government co-invention.
"Although USAMRIID performed extensive and critical screening and testing for Gilead, testing a compound and finding that it is indeed an effective antiviral compound does not qualify USAMRIID as a joint inventor of the compound," Leigh Callander, chief patent counsel for the U.S. Army Medical Research and Development Command, said in an email.
An independent organization that measures the cost-effectiveness of drugs said Gilead could be justified in charging up to $4,500 for a 10-day course of treatment for a single coronavirus patient. But advocates, citing a study by academic researchers on what it costs to make the drug, have said Gilead could break even by charging $1 per dose.
The Department of Health and Human Services, in response to emailed questions, said it was too early to discuss pricing of remdesivir but noted that the government has reimbursed hospitals and other providers for the costs of testing and treating people with no health insurance. For those with insurance, many insurance companies have waived patient co-payments for covid-19-related care and therapies, it said.
"The Trump Administration is committed to ensuring Americans have access to life-saving therapeutics and vaccines as we combat this pandemic," it said.
Gilead is donating the first 1.5 million doses to governments worldwide, which it said was enough for at least 140,000 patients through the end of May. More than half of that was targeted for U.S. patients. The drug is given intravenously in the hospital for five to 10 days. Gilead is investigating ways of making the drug in pill form, which could dramatically increase use - and sales - especially if the coronavirus lasts for years in the human population.
FULL ARTICLE @ THE HOUSTON CHRONICLE (via Washington Post)
www.chron.com/business/article/Taxpayers-paid-to-develop-remdesivir-but-will-15296173.php
(This article could be moved under coronavirus)










